World NTD Day 2020

World NTD (Neglected Tropical Diseases) Day 2020
30 January 2020 is the first ever World NTD Day, highlighting the Neglected Tropical Diseases (NTDs) still prevalent and affecting more than one billion people around the world. In 2017 the WHO NTD list included 17 infectious diseases, such as leishmaniasis, leprosy, dengue fever, rabies, and schistosomiasis (plus snake-bite, ectoparasites, and mycetoma).
NTDs are found primarily in low- and middle-income countries of Africa, Asia, and Latin America and mainly affect people living in poverty, who have limited access to clean water, sanitation and medicines. NTDs cause both death (mortality) and serious injuries (morbidity), such as blindness, limb deformity and loss, open wounds, and growth stunting. Sufferers face stigma and discrimination, as well as the missing of crucial time in school for education for children and at work earning an income for adults. These diseases have been historically underfunded and under-researched, but they are increasingly coming to the attention of funding agencies and scientists around the world, who want to change the lives of the one billion people affected by NTDs.
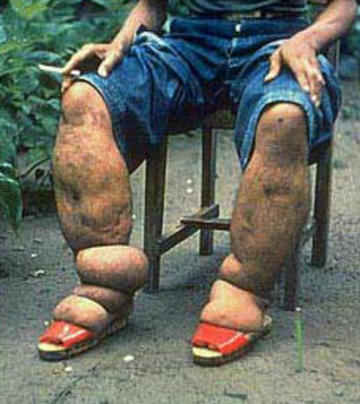
Lymphatic filariasis sufferer (caused by parasitic worms; credit CDC)
VALIDATE is part of this movement. Our members are scientists around the world working on vaccine development for leishmaniasis and leprosy - as well as melioidosis (which is so neglected it doesn't even make the WHO NTD list!) and tuberculosis (TB). At VALIDATE we're aiming to do our bit to end NTDs.
So, on this exciting first World NTD day, we spoke to VALIDATE Network Management Board member, Dr Alvaro Acosta-Serrano, who is a leishmaniasis researcher:

Hi Alvaro! Thanks for joining us on this historic first ever World NTD day. Your research concentrates on the NTD leishmaniasis. So what is leishmaniasis?
Leishmaniasis is a neglected tropical disease caused by a group of intracellular protozoan parasites known as Leishmania. It is estimated that at least 12 million people currently suffer from leishmaniasis across 88 countries. Cases of leishmaniasis are mainly concentrated in Asia, the Middle East, Latin America and Mediterranean countries. Leishmaniasis is a stigmatising disease that may lead to mental health problems (including depression) because of scarring. Leishmaniasis also affects some animals, such as dogs.
How do you get leishmaniasis and what are the symptoms?
Leishmania parasites are exclusively transmitted by sand flies, which can be found in both tropical and sub-tropical areas. Leishmaniasis can manifest as a cutaneous (or mucocutaneous) disease with different clinical presentations that may include skin ulcers and disfigurement. Some Leishmania species can also cause a visceral disease, which is estimated to be fatal in 95% of cases who don't receive treatment [read more about the symptoms of leishmanaisis here].
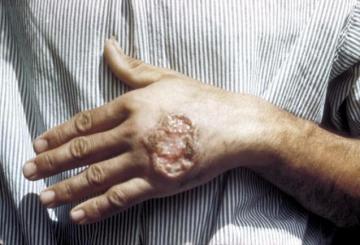
Skin ulcer caused by leishmaniasis (credit: CDC)
Where are we with a leishmaniasis vaccine and why is one important?
Unfortunately there is currently no available vaccine that is able to either protect or treat human leishmaniasis. There are some vaccines that are partially protective in pet dogs, but their efficacy is not high enough to disrupt the animal-to-human (zoonotic) transmission cycle.
There are also several experimental vaccine models that have some degrees of protection and mainly work by conferring a T cell immunity. New experimental leishmaniasis vaccine models include one that increases the levels of anti-Gal antibodies in serum (in which research my group had a little participation) and another one exclusively made of sand fly salivary proteins. Interestingly, it has been found that some salivary proteins are able to activate the immune system in ways that induce a protective T cell response, at least in experimental animals.
Creating a vaccine for leishmaniasis would be fantastic, but this has proven to be rather challenging due to several factors; the main one is perhaps the lack of funding allocated for vaccine development, but also difficulties in identifying protective antigens, lack of sand fly facilities and expertise to challenge vaccinated animal with an infectious bites, among others. In addition, leishmaniasis is a disease associated with poverty and conflict, both of which trigger massive human displacements that disrupt disease control programmes.
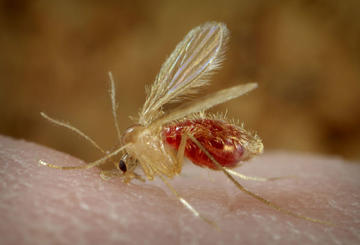
Leishmaniasis vector, the sand fly, taking a human blood meal
What is your leishmaniasis research about?
I have two main research programmes. The first deals with the control and transmission of cutaneous leishmaniasis in the Old World. This is a multidisciplinary programme that has been designed to lower the number of leishmaniasis cases in endemic areas. In recent years, cutaneous leishmaniasis has become hyperendemic in the Middle East as a consequence of the Syrian war and massive human displacement in the region.
One of the several interesting field observations from our research is that the status of the human skin microbiome appears to modulate the efficacy of the anti-leishmanial drugs. We have recently analysed the skin microbiota (skin flora) of a significant number of leishmaniasis patients and found that when the skin ulcers develop secondary infections, composed predominantly of opportunistic bacterial species (e.g. Staphylococcus), the patient becomes more resistance to drug treatment. I should point out that many leishmaniasis-endemic countries still use highly toxic antimonials as the first line of treatment, which are administered to the patients in intra-lesional (and painful) injections. After clearing the secondary infections the patient may need less antimonials injections or even self-heal. So we hope that these investigations will allow us to identify alternative drugs that will modulate the patient skin microbiome, and by doing so we may be able to minimise the use of toxic antimonials.
The second programme, which is a more basic science one, investigates how trypanosomes (parasites related to Leishmania but responsible for African sleeping sickness, which is another NTD) are able to colonise their tsetse fly vector and be transmitted by these insects. So we use a combination of genetics, biochemistry and microscopy to answer some of these fundamental and fascinating questions. This research may lead us to identify new transmission blocking vaccine candidates against trypanosomiasis.
How is VALIDATE helping in the battle to fight NTDs like leishmaniasis?
Although the development of a leishmaniasis vaccine may take some time, it will certainly speed up the current disease elimination programme. The role that networks like VALIDATE have in supporting research for the developing of new vaccines (or further strengthening current vaccine models) against intracellular pathogens like Leishmania is instrumental to achieve this goal. By bringing researchers together, providing crucial pump-priming funding, and supporting Early Career Researchers in our field to progress their careers, VALIDATE is helping to bring closer an effective vaccine against leishmaniasis.
A big thank you to Alvaro for speaking to us today. As well as leishmaniasis, VALIDATE researchers are also working to accelerate vaccine development for three other infectious diseases: melioidosis, leprosy, and tuberculosis (TB). You can find out more about these diseases, and the work VALIDATE is doing, on our Pathogens webpage.
Let's beat NTDs: For Good. For All.

Related stories: World Leprosy Day 2020 and 2019
Published 30 January 2020


